Welcome to the eleventh edition of FOI Clinical. Each week, we'll send you a briefing on outbreak news. When something urgent breaks, you'll get an alert the same day.
In this edition
Measles - Mpox - Chikungunya update - Rotavirus - Haemophilus influenzae - Legionellosis: early season signal - Mpox global update
National interest
Measles
As of April 16, 2026, there have been 1,748 confirmed cases of measles this year across 33 jurisdictions, up 34 from last week's 1,714. Nineteen outbreaks have been reported, and 94% of confirmed cases (1,637 of 1,748) are outbreak-associated. The weekly pace continues to slow.
- South Carolina: The outbreak centered around Spartanburg stands at 997 cases as of April 14, with no new outbreak-associated cases since March 17. The outbreak is set to be officially declared over on April 26, 42 days after the last case. However, a separate travel-associated case in an adult from Saluda County was reported April 14.
- California: 43 cases this year, arising from multiple smaller clusters around the state. San Francisco announced its first case since 2019 on April 15: an unvaccinated infant under 12 months who was exposed while traveling internationally.
- Utah: 405 cases this year (602 for the outbreak). No new cases reported this week.
- Texas: 4 new cases since last week, a slowdown compared to new cases reported in March and earlier in April.
- Oregon: 3 new cases have been reported weekly for each of the last three reporting weeks. The state has reported 20 cases this year.
Mpox
Mpox cases continue to accumulate in 2026 at a pace well above last year. Through MMWR week 14, there have been 453 cases reported through the National Notifiable Disease Surveillance System (NNDSS), compared to 255 at the same point in 2025, a 1.8x increase, up from 1.7x the prior week. California is averaging 14.5 mpox cases per week this year, more than double the rate from the same period in 2025.
The majority of U.S. cases remain clade IIb, the strain responsible for the 2022 global outbreak, circulating at low but persistent levels primarily among unvaccinated or partially vaccinated men who have sex with men (MSM).
However, clade Ib, the strain driving the ongoing outbreak in Central and Eastern Africa, is now present in the United States. Sixteen clade I cases have been confirmed nationally since November 2024, seven of them in California, including San Francisco's first case, an unvaccinated resident who was hospitalized after close contact with an international traveler. More than a quarter of all U.S. clade I cases were diagnosed in March 2026 alone.
CDC continues to assess the risk of clade I mpox to the general public as low and to MSM as low to moderate. Vaccination with JYNNEOS is believed to be effective against clade Ib.
Rotavirus: elevated activity amid vaccination decline
Rotavirus is surging across the United States, with wastewater data showing sustained high levels since January. Data from WastewaterSCAN (Stanford/Emory) shows rotavirus RNA was detected in 98% of all sampling sites in March 2026, with concentrations rising every month since December, up 43% in January, 42% in February, and 29% in March. Of 147 monitored sites, 101 (69%) are in the high category for rotavirus detection.
Rotavirus is not nationally notifiable, so it does not appear in NNDSS data. Wastewater surveillance and the CDC's NREVSS laboratory detection system are the primary data sources. NREVSS data corroborate the wastewater signal: national rotavirus percent positivity has climbed from ~1% in late December to ~7.5% in mid-April 2026, a sustained four-month acceleration, with testing volume steady at roughly 3,000–3,800 PCR tests per week.
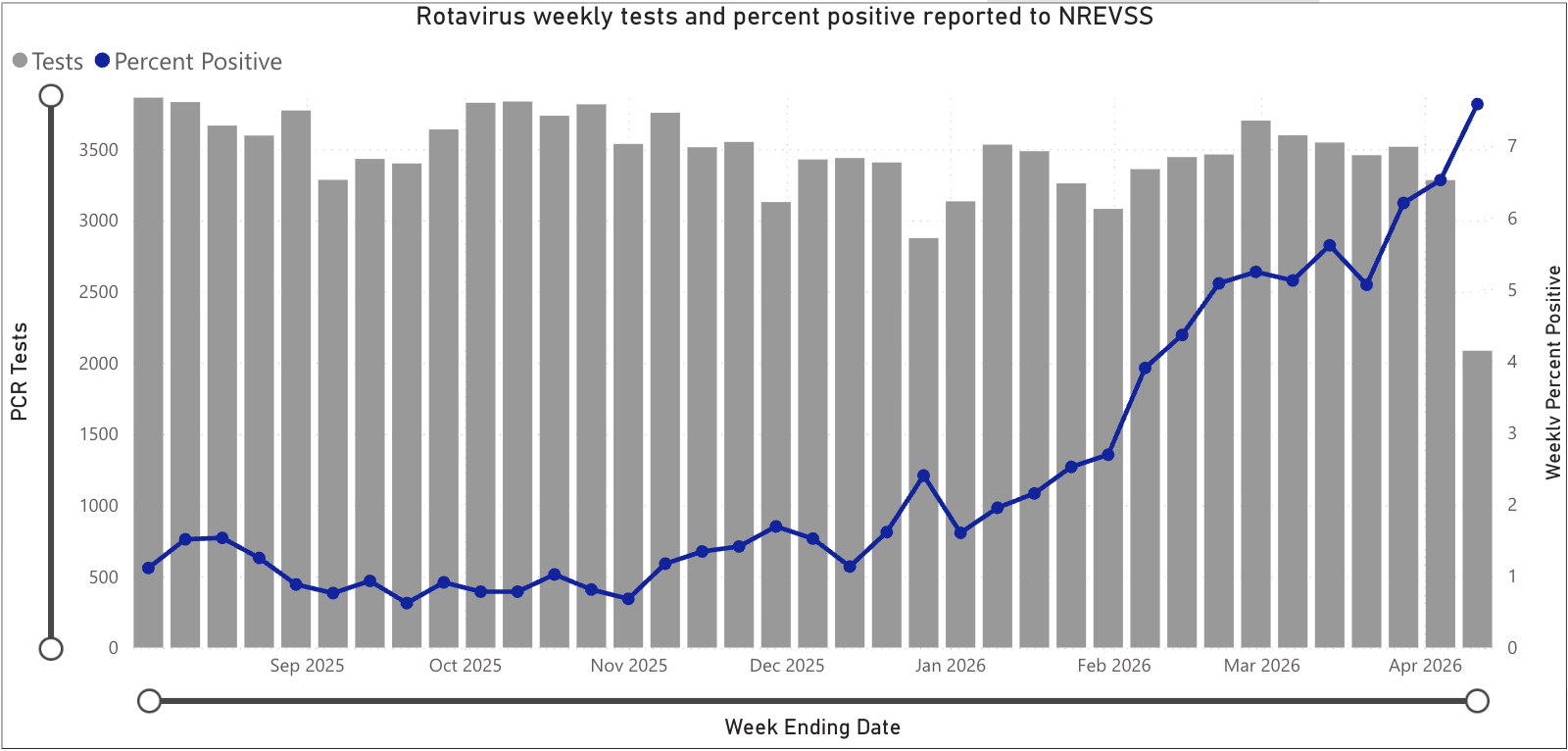
The surge comes as rotavirus vaccination coverage continues to decline. Nationally, 73.8% of children have completed the full rotavirus vaccine series, a figure that has dropped every year for the past eight years. The vaccine prevents an estimated 40,000 to 50,000 hospitalizations every year among infants and young children. Most children being hospitalized for rotavirus are either too young to be vaccinated, have not completed the full series, or are unvaccinated.
In January 2026, the CDC moved rotavirus from a universal recommendation to "shared clinical decision-making", meaning the vaccine is no longer routinely recommended for all children, but rather discussed between clinicians and parents on a case-by-case basis.
Rotavirus causes acute-onset vomiting and watery diarrhea, primarily in children under 5. It is highly contagious and spreads through the fecal-oral route. Severe cases can lead to dehydration requiring hospitalization; before the vaccine was introduced in 2006, rotavirus caused approximately 410,000 physician visits, more than 200,000 emergency department visits, 55,000–70,000 hospitalizations, and 20–60 deaths annually in the U.S., according to CDC’s textbook on the vaccine-preventable diseases.
Haemophilus influenzae update
Invasive Hib serotype b in children under 5 has ticked up to 10 cases year-to-date, more than double the 4 cases seen at the same point in 2025. The numbers remain small in absolute terms, but the ratio continues to climb week over week. As covered in Issues 8 and 10, this tracks with declining Hib vaccination coverage (now 77.6%) and renewed clinical attention to a disease that had been largely eliminated by routine childhood immunization.
Legionellosis: early season signal
Legionella cases spiked in MMWR week 14, with 41 cases reported nationally, nearly double the historical average of 24 for this time of year. The seasonal baseline for week 14 has been rising year-over-year (15 → 21 → 28 → 31 from 2022–2025), and this week's count exceeds even that upward trend.
Reporting to NNDSS is uneven, so single-week numbers must be considered in the context of other epidemiological observations, including year-to-date trends, which show reported legionellosis cases (1,344) are running below last year (1,743 at the same point, 0.8x ratio). Early warning signals lose value if acted on only in retrospect; this spike is flagged here pending confirmation from subsequent weeks of reporting.
Legionellosis typically peaks in late summer and early fall (August–October), driven by warm-water conditions in cooling towers, hot tubs, and plumbing systems. Legionellosis is a bacterial lung infection caused by Legionella species, most commonly L. pneumophila. It is not spread person to person–people become infected by inhaling aerosolized water droplets contaminated with the bacteria. Common sources include cooling towers, building water systems, hot tubs, and decorative fountains. Legionnaires' disease, the more severe form, presents as pneumonia and can be fatal, particularly in older adults, smokers, and immunocompromised individuals. Reported cases have risen substantially since the early 2000s, and the disease is considered significantly underdiagnosed. About 1 in 10 people who develop Legionnaires' disease will die from the illness.
This year marks the 50th anniversary of the discovery of legionella.
Chikungunya update
Chikungunya remains elevated, as reported in last weeks FOI Clinical, but case counts appear to be stabilizing. Through MMWR week 14: 139 cases nationally (5.1x prior year), with Florida accounting for 129 (93%). The weekly count has slowed to 1 case in week 14. NNDSS reporting lags can affect these counts, so these observations are preliminary.
The ongoing Cuba outbreak continues to drive travel-associated cases into Florida. No new locally acquired cases have been identified since the single December 2025 case in Miami-Dade County.
International interest
Mpox
Clade Ib mpox continues to expand geographically. Denmark registered its first suspected clade Ib case on April 14, a person likely infected through sexual contact abroad who developed mild symptoms after returning home. Danish health authorities said the case does not warrant a change in their risk assessment for the country.
Globally, the clade I mpox outbreak has produced over 53,000 confirmed cases since January 2024, including more than 150 deaths, the vast majority in the Democratic Republic of the Congo. The true death toll is likely considerably higher given limitations in laboratory confirmation across affected areas. A declining trend in new cases has been reported since May 2025.