Welcome to the first edition of FOI Clinical. Each week, I'll send you a briefing on outbreak news. When something urgent breaks, you'll get an alert the same day.
In this edition
Notable measles clusters - Shift toward influenza B - Pertussis trends - Meningitis in Illinois - Tularemia in Oklahoma - Mumps in Maryland - Nipah in India and Bangladesh
National Interest
Measles
Measles outbreaks continue around the country, with 2026 on track to become another banner year. Measles incidence is the highest it's been in decades, with over 340 cases reported in December and another 721 in January.
Several notable outbreaks are underway. The outbreaks highlighted below are not a comprehensive list but rather a selection of prominent active clusters worth keeping in mind.
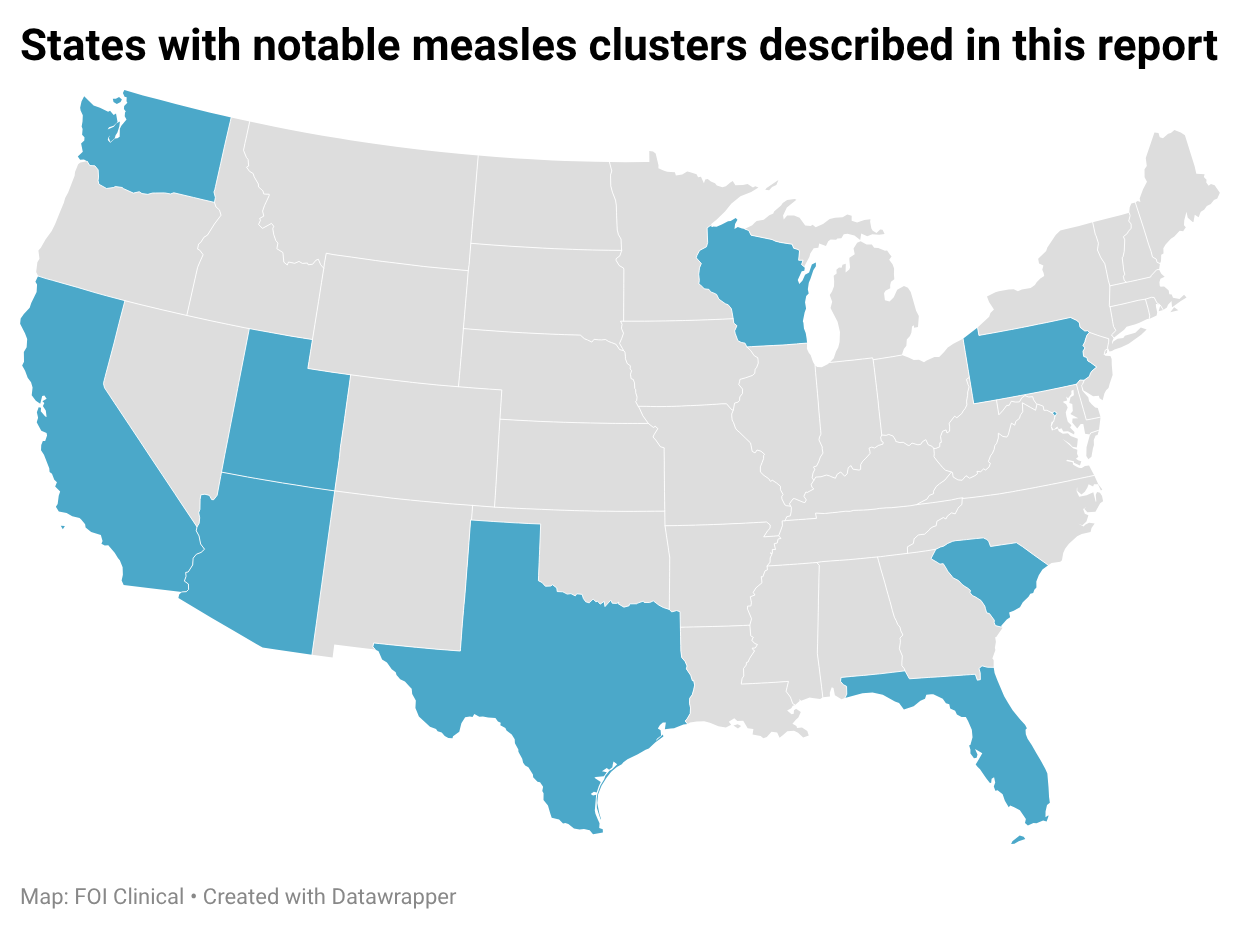
- South Carolina: A multi-county outbreak in South Carolina has grown to 933 cases, including 68 confirmed the week of February 1st. The Upstate region is most heavily affected, and a majority (859) of cases are in people who are unvaccinated.
- Arizona/Utah: An outbreak on the Arizona/Utah border has grown to hundreds of cases, including 251 on the Utah side and 254 on the Arizona side. A combined 18 cases were recorded during the most recent reporting week.
- Collier and Alachua, Florida: Around 50 suspected cases have been reported in association with Ave Maria University. The University of Florida has also reported two public exposures.
- Lancaster, Pennsylvania: Five cases were announced on February 3rd. All five cases were in people who are unvaccinated.
- Multiple locations, California: Multiple counties are reporting measles cases: Los Angeles, Orange, San Bernardino, Riverside, and Shasta. Of particular note are several instances of public exposures at Disneyland, including three people who visited in late January and a second instance reported earlier this week. The California Department of Public Health issued a press release urging residents to get vaccinated.
- Washington, D.C.: Multiple confirmed cases in the city between January 21st and February 2nd generated a large number of public exposures, including the emergency department at Children's National Medical Center, as well as several regional transit hubs.
- Clark County, Washington: A cluster of seven cases has been reported, with a local high school and medical clinic exposed.
- Dilley Immigration Processing Center, Texas: Two cases were recently reported in detainees. Congregate settings like this are very dangerous for measles outbreaks. The virus can move quickly and be difficult to control in these settings.
- Milwaukee, Wisconsin: A person flew from Phoenix to Milwaukee while infectious with measles, apparently against isolation orders. Measles has also been detected in wastewater in Walworth County.
The Pan American Health Organization will meet in April to evaluate the United States' measles elimination status. It's likely we will lose our status, as Canada did in November and the UK in January.
Shift toward influenza B
Influenza activity has declined in most areas of the country, following an early January peak. However, the proportion of flu cases that are influenza B is rising as we head further into the spring months. Although influenza B is often regarded as milder compared to flu A, studies have shown that there is no significant difference in severity.
FOI Clinical visualization of CDC FluView data
Pertussis
Pertussis activity is elevated in many areas of the country, though it has declined since its fall 2024 peak. A typical month in 2022 would have seen fewer than 200 cases reported. But now, over 600 per month is not uncommon.
Pertussis is an under-reported disease, and so numbers are best understood as trends or estimates rather than a comprehensive accounting of burden. Recent data may be incomplete.
Certain regions of the country are more heavily affected than others. All numbers are rounded for ease of reading.
- The Mid-Atlantic saw a notable climb from 80 cases in October to over 120 in December; data for January seem incomplete, likely due to a reporting lag.
- The East North Central Midwest has been steady in the 85-120 range, while the West North Central Midwest is in the 15-40 range.
- The South Atlantic remains elevated in the 85-120 per month range, though there was a notable spike over the summer with >200 monthly cases reported.
- The East-South Central region has been stable with around 20-50 reported cases per month.
- The Mountain West stands out with 90 to 130 cases per month in recent months, driven by surges in Arizona and Colorado.
- The Pacific region has also seen a recent spike, climbing from 40 to 60 cases per month.
- Activity in New England remains relatively low.
FOI Clinical analysis of NNDSS data
According to data from 2024, recent cases are most commonly reported in children 11 to 19 years of age. When adjusting for age, infants are most affected. Infants are also most likely to be hospitalized. Cases are not exclusively in people who are unvaccinated; 26% of cases had completed their primary series. In 2024, there were 10 deaths from pertussis.
Pertussis vaccine coverage among kindergarteners has declined from around 95% nationally in 2019 to 92% in 2024. The national goal (which does not directly correspond to school coverage but is still a useful reference point) is for 90% of children to receive 4 or more doses of DTaP by their second birthday. (This map is interactive when opened in the browser.)
FOI Clinical visualization of CDC's SchoolVaxView data
Regional News
Meningitis in Illinois
Chicago has reported at least seven cases of meningococcal disease and two deaths in adults in January 2026. The city typically sees 10–15 cases in a year.
Meningococcal disease can progress from mild flu-like symptoms to life-threatening meningitis or bloodstream infection within hours. Even with antibiotics, 10–20% of cases are fatal. It spreads through prolonged close contact. There has been a notable increase in serogroup Y incidence in recent years.
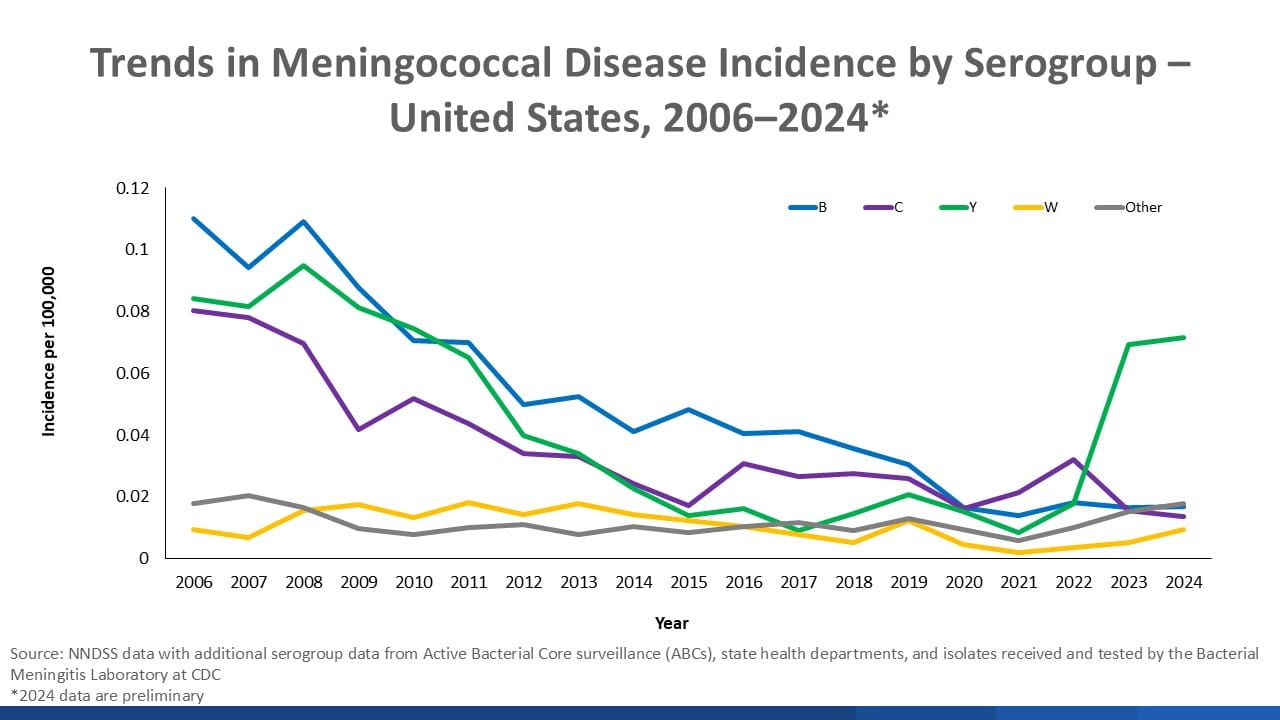
The CDC recently narrowed its meningococcal vaccine recommendation for children, moving from a universal recommendation to shared clinical decision making. The American Academy of Pediatrics continues to recommend routine vaccination against meningococcal disease.
Tularemia in Oklahoma
Notifiable disease data shows a spike in tularemia in Oklahoma late last year, with 10 cases in November and three in December. This is above the typical incidence of two to three cases per month during the off-season. No cases were reported in January. Oklahoma's Department of Health did not respond to a request for comment.
Tularemia is an uncommon bacterial infection caused by Francisella tularensis. It is most often acquired through tick and deer fly bites, handling infected animals (particularly rabbits and rodents), or contact with contaminated water or soil.
Cases peak in the summer months, with national totals typically ranging from five to ten per month. The disease can present in several forms depending on the route of infection, ranging from skin ulcers and swollen lymph nodes to pneumonia, and can be serious if not treated promptly.
Tularemia has been reported in most areas of the country, with the South-Central region the most commonly affected.
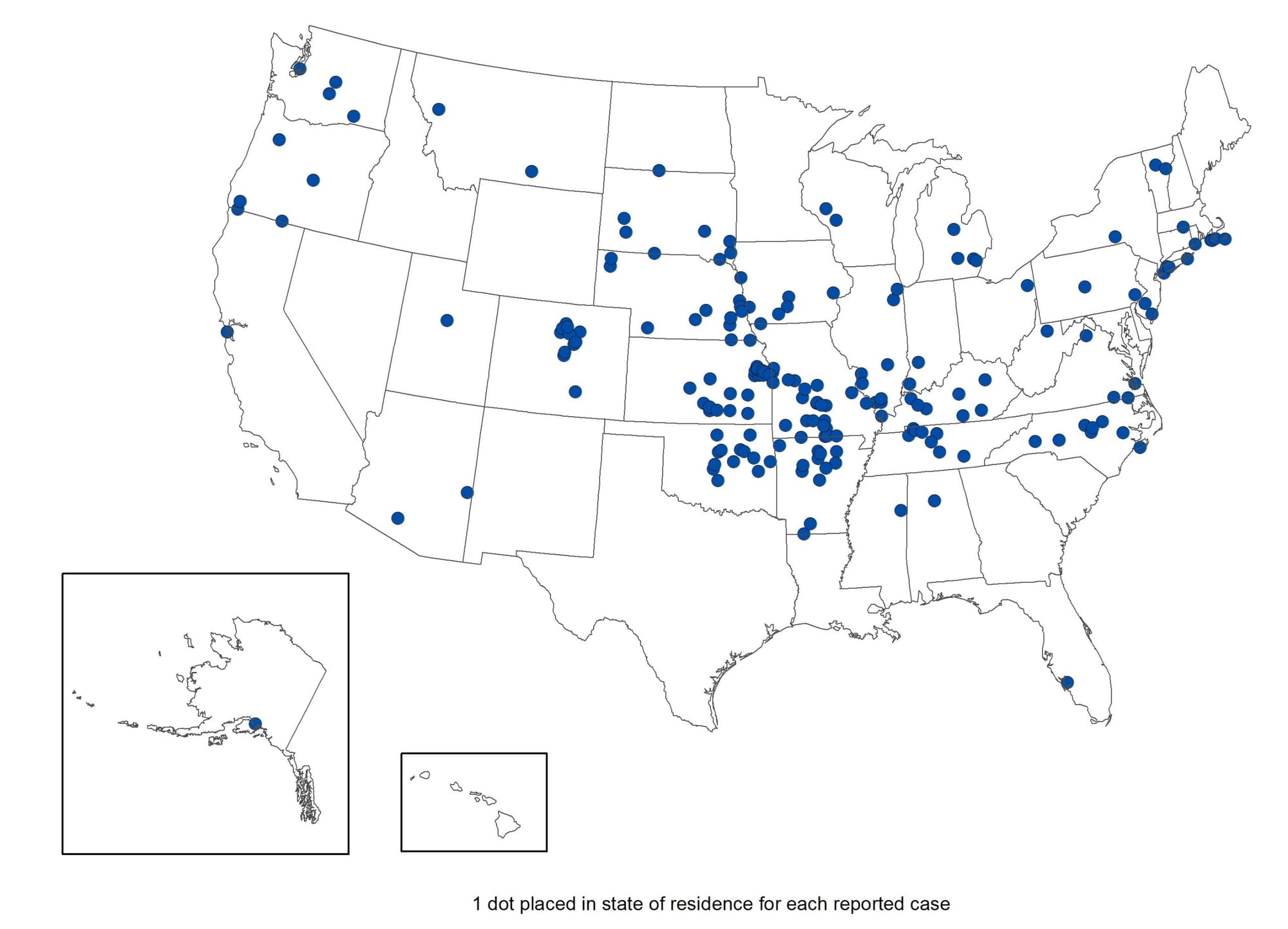
Mumps in Maryland
Late-breaking news: There is an increase in mumps cases in the Baltimore metro area, with 10 confirmed and 4 probable cases reported, mostly in adults. I am working to obtain more information.
International News
Nipah Virus
The World Health Organization (WHO) has issued two Disease Outbreak News reports about cases of Nipah.
- India reported two cases in West Bengal State in late January. Both cases were in healthcare workers at the same facility; though the source of infection is not specified, occupational exposure seems likely. Nearly 200 contacts were traced and tested negative. This is the higher risk of the two outbreaks, but at this point it appears contained.
- Bangladesh reported one case who developed symptoms in mid-late January. The person "had a history of consuming raw date palm sap," which is a known source of Nipah virus infection. The case died shortly after hospital admission. All 35 contacts traced have tested negative.
The risk of these events impacting the United States is very low, but the outbreaks have made headlines because Nipah is thought to be a virus with pandemic potential (see e.g., WHO).
